Understanding Why Areolar Incisions Are Avoided in Breast Augmentation by Dr. David Rapaport
January 29, 2026
Breast augmentation is one of the most common cosmetic surgeries performed worldwide, with millions of women seeking to enhance their appearance every year. However, the surgical approach and incision placement can significantly affect surgical outcomes and potential complications. One critical consideration is why many surgeons, including Dr. David Rapaport, shy away from making incisions through the areolas during breast implant procedures. This blog post explores the core reasons for this practice, focusing on the risks of capsular contracture and bacterial contamination, and on the evolution of surgical techniques designed to minimize these risks.
What is Capsular Contracture?
The Formation and Impact of Capsular Contracture
Capsular contracture is one of the most well-known complications associated with breast implants. It refers to the process where the scar tissue that naturally forms around the implant tightens and squeezes the implant. This tightening effect can make the breast feel abnormally hard, sometimes as hard as a rock, despite the implant itself remaining soft and intact. The firmness and discomfort caused by capsular contracture can significantly affect the aesthetic results and may require corrective surgery.
Causes of Capsular Contracture: The Role of Low-Grade Infection
A major underlying cause of capsular contracture is believed to be a chronic low-grade infection. Unlike acute infections that cause fever, pus, and require immediate medical intervention, these infections are subtle and persistent. They involve bacteria that adhere to the implant surface, forming protective layers known as biofilms. These biofilms shield bacteria from the body’s immune system and antibiotics, leading to a slow, ongoing inflammatory response.
Biofilms: The Hidden Threat in Breast Augmentation
Understanding Biofilms in Medical Implants
Biofilms are complex colonies of bacteria that grow on various surfaces, especially synthetic materials like implants and intravenous lines. This field of study has been evolving for over 30 years, and it is now understood that biofilms play a critical role in many medical device-related infections. These bacterial layers are notoriously difficult to eliminate and can cause persistent inflammation without the typical signs of infection such as fever or elevated white blood cell counts.
Biofilms in Breast Implants and Their Consequences
In breast augmentation, biofilms can form on the surface of the implant, leading to chronic inflammation that contributes to capsular contracture. Because these bacteria are not overtly aggressive, they do not cause acute infection symptoms but are sufficient to trigger scar tissue hardening. This subtle but damaging process explains why preventing bacterial contamination during surgery is crucial.
Why Areolar Incisions Increase Infection Risk
Anatomy of the Areola and Bacterial Presence
The nipple and areola complex have ducts that provide a natural passageway from the skin surface to the breast tissue. These ducts harbor bacteria, similar to how the inside of the nose contains microbes despite external cleaning. Even with thorough skin preparation before surgery, bacteria inside these ducts cannot be completely sterilized.
Risk of Bacterial Leakage During Surgery
When an incision is made through the areola, these hidden bacteria can leak out and contaminate the surgical site and implant surface. This contamination increases the risk of biofilm formation and, consequently, capsular contracture. It is for this reason that surgeons prefer to avoid areolar incisions whenever possible.
The No-Touch Technique: Minimizing Contamination in Breast Augmentation
What is the No-Touch Technique?
Over the past 15 to 20 years, breast augmentation surgery has evolved with the development of the “no-touch” technique. This approach focuses on minimizing the implant’s exposure to bacteria during surgery by avoiding direct contact between the implant and the skin or gloves.
How the No-Touch Technique Works
In practice, the no-touch technique involves several critical steps:
- Avoiding incisions through the areola to reduce exposure to ductal bacteria.
- Using sterile barriers such as a teederm (a sterile drape) over the nipple and areola complex to prevent bacterial leakage.
- Handling implants with instruments or sleeves rather than directly with gloves.
- Ensuring the incision site is as clean and protected as possible.
By implementing these measures, surgeons significantly reduce the risk of bacterial contamination and subsequent biofilm formation on the implants.
Additional Considerations in Surgical Incision Placement
Alternative Incision Sites in Breast Augmentation
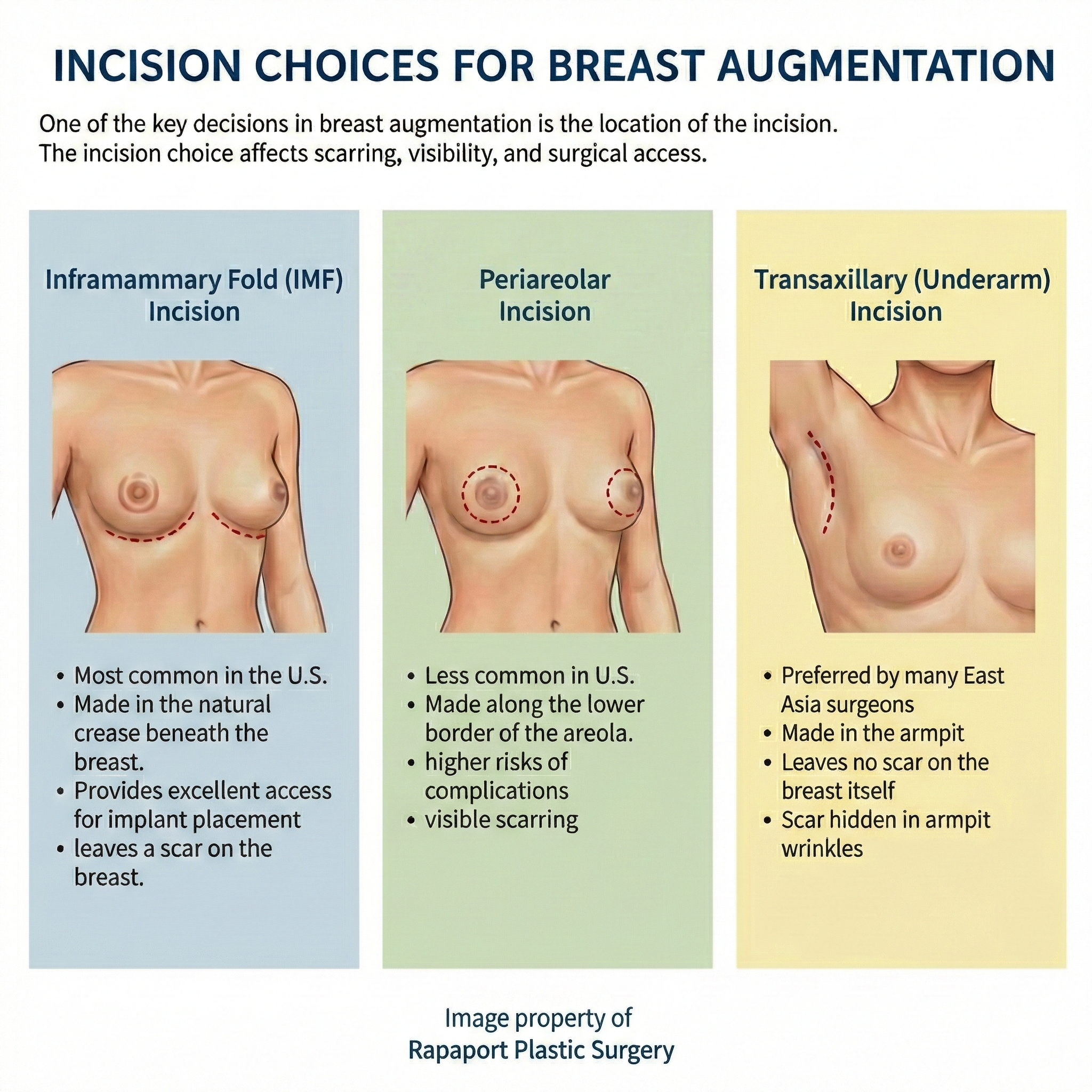
To reduce the risk of capsular contracture related to bacterial contamination, surgeons often opt for incision sites away from the nipple-areola complex. Common alternative approaches include:
- Inframammary fold incision: placed in the crease under the breast.
- Transaxillary incision: made in the armpit area.
- Transumbilical incision: through the navel (less common).
Each of these sites avoids the bacterial-rich ducts of the areola, lowering the risk of contamination.
Balancing Aesthetic Outcomes and Surgical Risks
While areolar incisions may offer more discreet scarring, the increased risk of capsular contracture and implant complications often outweighs the cosmetic benefit. Surgeons and patients must discuss the trade-offs between scar visibility and long-term implant health.
Conclusion: Prioritizing Patient Safety in Breast Augmentation
Breast augmentation is a highly effective cosmetic procedure, but success depends on meticulous surgical technique and infection prevention strategies. Avoiding areolar incisions is a key decision driven by the desire to minimize capsular contracture risk caused by hidden bacterial biofilms. The adoption of the no-touch technique and careful incision placement represents advances in surgical practice that improve patient outcomes and implant longevity.
By understanding these factors, patients can make informed decisions and have realistic expectations about their breast augmentation journey. Always consult with a board-certified plastic surgeon who prioritizes both aesthetic results and patient safety.
If you’re interested in learning more about breast augmentation techniques or would like to schedule a consultation at our New York office, contact us today.